This information is for health professionals and service providers.
This section of the MND Connect website provides evidence based and best practice information for health, disability and aged care providers working with people living with motor neurone disease. The aim is to help those involved in MND care and support to:
- assess the needs of the person with MND and their carer
- get evidence based and best practice MND information
- make referrals to the right provider at the right time
- provide a coordinated, multidisciplinary team approach to MND care.
Statement on sources of literature
There is no ‘recipe’ for managing MND, however, evidence based and best practice information constitutes an effective tool for health professionals and service providers in managing clients with MND.
Research is evolving rapidly in the area of MND care and this web site endeavours to keep health professionals and service providers ‘up to date’ with research related to MND care, therapies, interventions and guidelines.
Where evidence is not available then best practice information has been sourced from information published or presented by experts and people experienced in MND care management.
MND Australia identified the need for a national ‘one stop shop’ motor neurone disease information website to facilitate and promote best practice care and support for all people with a diagnosis of MND in Australia. In November 2009 MND Australia received funding from the Australian Department of Health and Ageing for the "Living Better for Longer Project: facilitating a coordinated multi/interdisciplinary approach to MND Care in Australia through ‘one stop shop’ e-resources".
The objective of the project was to support health and community professionals to assist people living with motor neurone disease to live better for longer through the provision of easily accessible, comprehensive, up to date and evidence based or best practice online information to address needs and symptoms related to MND. The project was developed by a team of people experienced in MND care and the needs of people living with MND. Development commenced in November 2009 and the MNDcare website went live on 21 June 2010.
Since then the introduction of the national disability insurance scheme (NDIS) has changed the service provision landscape in Australia. Timely, accessible and consistent information is vital in fostering choice and control for people living with MND and enabling them to access services and supports to meet their individual needs and achieve their identified goals.
These changes highlighted an urgent need to update the MNDcare website to address the changed service system priorities since the introduction of the NDIS. This included the need to identify and address gaps related to MND specific information for mainstream organisations and service systems that may have little or no experience of supporting people with a rapidly progressing and complex disability such as motor neurone disease.
In November 2019 MND Australia received a three year grant from the Information, Linkages and Capacity Building (ILC) National Information Program Funding Round 2019-2022 to deliver the MND Connect Project - Connecting people impacted by motor neurone disease to consistent, quality information to foster choice and control, and to relevant, appropriate and inclusive services and supports responsive to their needs and expectations.
MND Connect supports the provision of a national model of good practice connecting people living with MND and service organisations to immediate, accessible and consistent MND specific information to enhance independence and social and community participation.
There is no known cause for MND (except in a very small number of genetic cases), no effective treatments and no cure - yet. Progression of MND is usually rapid and relentless creating high levels of disability and a consequent need for a wide range of supports based on the person’s changing and progressing needs. The needs of people diagnosed with MND are complex and vary from person to person. MND may start in different areas of the body and progress in different patterns and at different rates. There is no 'recipe' for managing MND, but the following approach to MND care provides a framework for management.
A person living with MND needs:
- information and support:
- from the onset of symptoms
- during the often protracted period of uncertainty prior to diagnosis
- ongoing in response to diagnosis, progressive deterioration and impact on family life
- access to the skills of experts with an understanding of MND from a variety of services including; medical, nursing, allied health, palliative care, MND associations, disability and aged care, to ensure optimal care and support from diagnosis through to bereavement.
The MND Care approach assists Australian health professionals and service providers to provide a person-centred approach to help people living with motor neurone disease live better for longer.
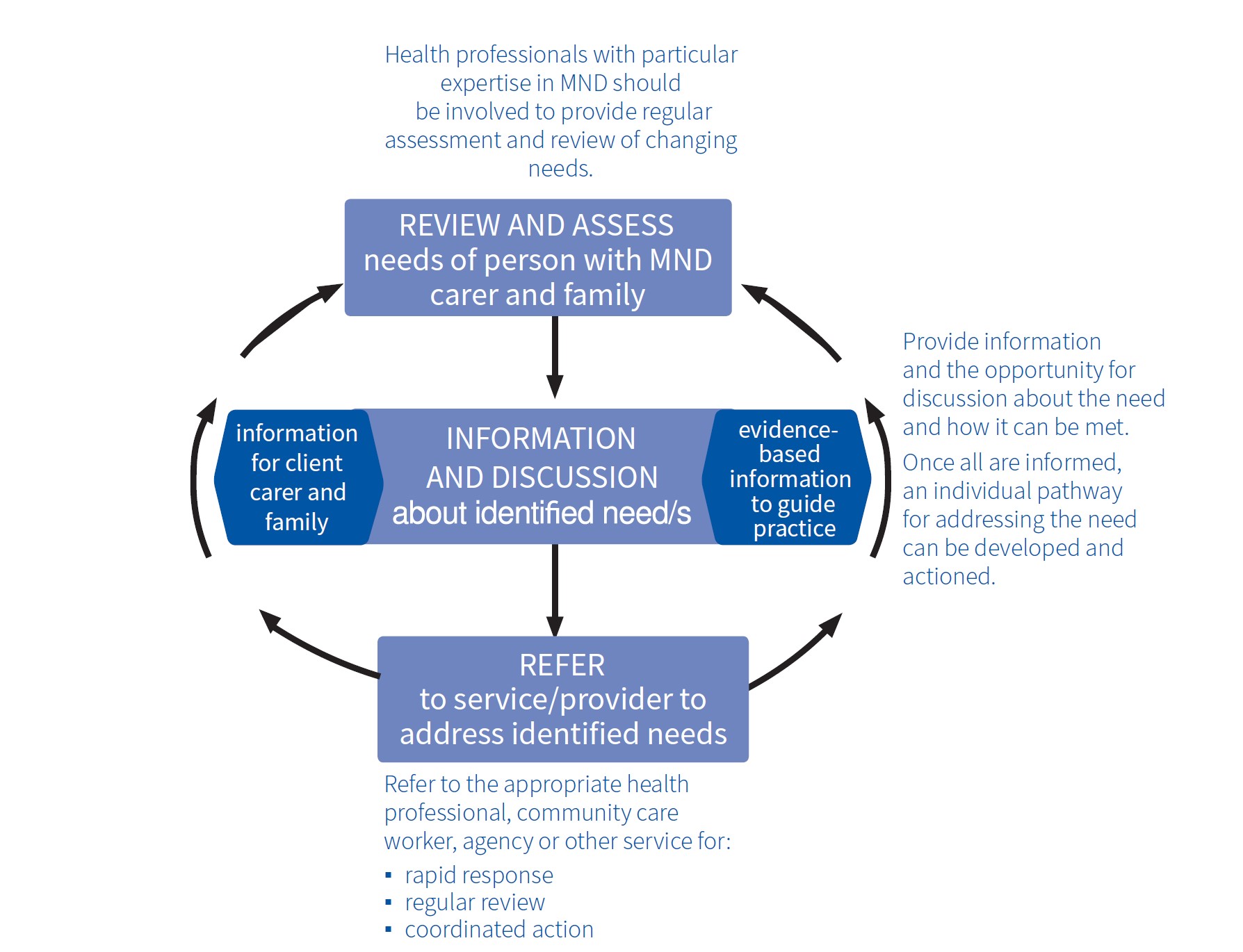
The MND care approach
1. Review and access
The effects of MND – initial symptoms, rate and pattern of progression, and survival time after diagnosis vary significantly from person to person. Regular review and assessment of changing needs of the person living with MND as well as their family and/or carer is therefore vital in managing symptoms, providing timely interventions and maintaining quality of life. Regular review and assessment is also important to ensure timely access to services and supports responsive to the needs and expectations of people living with MND.
Non‐pharmacological management strategies improve quality of life and prolong survival in MND, and in absolute terms these benefits are greater than disease‐modifying therapy with riluzole. Measures that may prolong survival include multidisciplinary clinic care, NIV, enteral feeding and a moderate exercise programme (Simon et al 2015).
2. Information and discussion
Information and discussion are at the centre of MND care. Quality MND specific evidence based information for health professionals and service providers to guide practice will enhance the ability of relevant supports and services to respond to the needs and expectations of people with MND.
The provision of trusted and accessible information to people living with MND and their families, when they are ready and ask for it, is vital in supporting people to play an active role in decision making. The provision of high quality information and the opportunity for discussion is also key in supporting choice and control and planning ahead to enhance quality of life, independence and social and community participation.
Accessible information and links to further related resources for people living with MND, their family and carers to enhance and support discussion and decision making is available on this website. Printed resources are available from the MND Associations.
3. Refer
As MND progresses and the person's condition changes over time, the composition of the health professional team, services and supports will also change to ensure their physical and psychosocial needs are met.
Referral to the right health professional and/or service at the right time is vital to ensure:
- rapid response
- coordinated action
- regular review
- access to timely interventions and assistive technology
Information and Referral Guidelines:
Information and discussion:
The National Institute for Health and Care Excellence (NICE) 2016 guidelines - see recommendation:
1.2 Information and support at diagnosis
Referral:
The National Institute for Health and Care Excellence (NICE) 2016 guidelines - see recommendation:
1.1 Recognition and referral
The International Alliance of ALS/MND Association's Fundamental Rights for People living with ALS/MND
state that people living with ALS/MND have the right to:
- the highest quality care available within their healthcare system
- the highest quality treatment available within their healthcare system
- information and education that will enable them to play an active role in making decisions
- choice with respect to:
- health and support workers who are providing treatment or advice
- the location where care takes place, and
- the type of treatment or support that is provided
- end of life choices which include the right to accept, refuse, or discontinue treatment or intervention within the legal framework of one’s own country
- provide input on the healthcare and support systems, including policy-making, care delivery and the implementation of medical research procedures and protocols
- the best quality of life possible
- live without discrimination
- confidentiality and privacy regarding their personal information
- receive any available governmental or other economic remuneration, benefits, and entitlements
- have access, upon diagnosis, to:
- up-to-date education about clinical genetics in ALS/MND
- genetic counselling
- genetic testing
- safeguards against genetic discrimination
- subject to education and counselling, blood relatives should also be given the same access, where relevant
A timely, coordinated, multidisciplinary team approach is vital for people living with MND and their carer. Early referral to one of the specialist MND multidisciplinary clinic is important to confirm diagnosis, provide access to clinical trials, where appropriate and available, and to support access to evidenced based interventions to manage symptoms and improve quality and length of life.
Most people, however, will also be supported on a day to day basis by their local community based health, palliative, disability and/or aged care professionals and providers. There may therefore be many people involved in providing care and support to the person with MND and their family, often from a range of services and organisations.
Identifying a key worker, such as a support coordinator or MND clinic nurse coordinator, as a main point of contact will help in ensuring a coordinated multi/interdisciplinary care approach to facilitate regular review and assessment, timely referrals and organisation of team meetings.
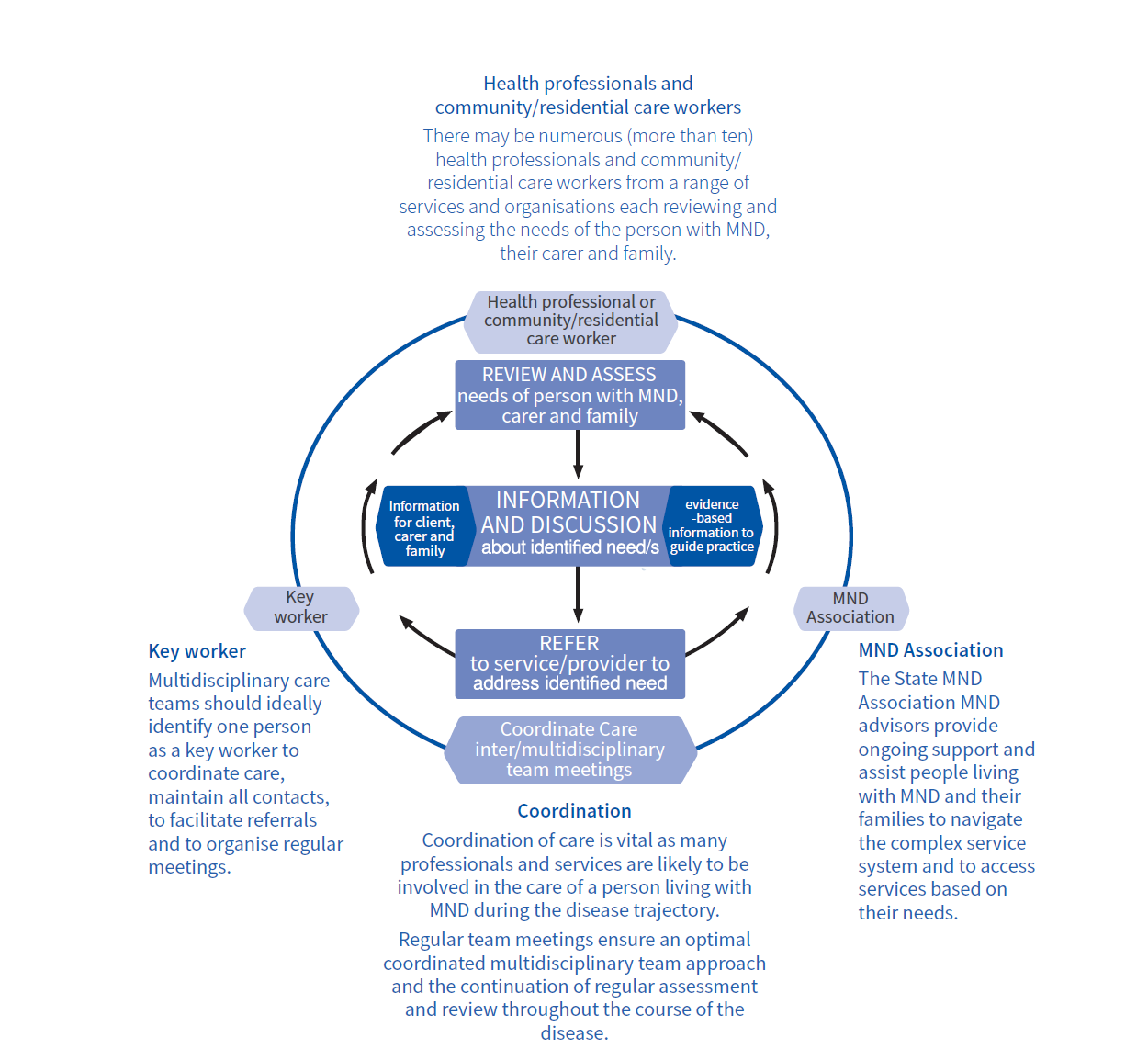
Given its progressive and debilitating nature and the lack of cure, management of MND is focused on symptomatic relief, optimising quality of life and timely palliative care involvement. Early referral to a dedicated MND multidisciplinary clinic is important to address the multiple facets and highly specific and complex individual care needs of this group (Lau et al 2018).
There is no quality randomised controlled trial evidence in a Cochrane Systematic Review to demonstrate any benefit or harm for multidisciplinary care in MND.
However the authors concluded that the nature of MND makes it difficult to research clinically accepted or recommended practice, regardless of the level of evidence supporting the practice. It would not be ethical, for example, to design a placebo‐controlled trial for treatment of pain in MND or to withhold multidisciplinary care where such care is available. It is therefore highly unlikely that there will ever be classically designed placebo‐controlled RCTs in these areas.
The absence of proof that multidisciplinary care is effective must not be interpreted as proof that this approach is ineffective. There are multiple, well-defined interventions, such as nutritional support and respiratory support, and interventions by physical, occupational and speech therapists which have individually had significant impact on disease course (Ng et al 2017).
In the absence of a curative therapy, the management of MND remains focused on symptom control, with the primary aim of maintaining quality of life. Evidence‐based management guidelines advise a multidisciplinary model of care, led by a neurologist and clinical nurse consultant working together with physical therapists, occupational therapists, speech pathologists, respiratory physicians, palliative care physicians, gastroenterologists, psychologists and social workers to guide patient management, and such an approach has profoundly impacted on the patient's quality of life and survival (Simon et al 2015).
Multidisciplinary care guidelines
Shoesmith et al 2021, Canadian best practice recommendations for the management of amyotrophic lateral sclerosis: From key points: 'Management of patients living with amyotrophic lateral sclerosis (ALS) requires specialized multidisciplinary holistic care'. See also: table related to multidisciplinary care.
The National Institute for Health and Care Excellence (NICE) 2016 guidelines - see recommendation: 1.5 Organisation of care
Andersen et al 2012, EFNS guidelines on the Clinical Management of Amyotrophic Lateral Sclerosis (MALS) – revised report of an EFNS task force - Multidisciplinary care recommendations:
- Multidisciplinary care should be available for people affected by ALS. Attendance at multidisciplinary clinics may extend survival, decrease medical complications (level B) and improve quality of life (level C).
- The following specialists should be part of or readily available to the multidisciplinary clinic team: neurologist, respiratory physician, gastroenterologist, rehabilitation medicine physician, social counsellor, occupational therapist, speech therapist, respiratory therapist, specialized nurse, physical therapist, dietitian, psychologist, dentist and palliative care physician (GCPP).
- Patients should generally be reviewed every 2–3 months, although they may require more frequent review in the months following diagnosis or in the later stages of disease, and less frequent review if their disease is progressing slowly. The patient support team should maintain regular contact with the patient and relatives between visits (GCPP).
- Ideally, the patient should be followed by the same neurologist liaising closely with the patient’s primary care physician (family general practitioner) (GCPP).
- Effective channels of communication and co-ordination are essential between the hospital-based multidisciplinary clinic team, the primary healthcare sector, the palliative care team and community services (GCPP). (Andersen et al 2012)
Miller et al 2009, American Academy of Neurology (AAN) update: The management and care of the patient with amyotrophic lateral sclerosis (ALS): Multidisciplinary care, symptom management, and the treatment of cognitive/ behavioral impairment:
Recommendations:
Specialized multidisciplinary clinic referral should be considered for patients with ALS to optimize health care delivery (Level B) and prolong survival (Level B), and may be considered to enhance quality of life (Level C).
A palliative approach is required following a diagnosis of MND to ensure that early discussions around future care management decisions and advance care planning are held and optimal symptom management for the person with MND and their family is achieved.
- the aim is to assist people with MND to maintain quality of life and also to support MND carers to maintain their own health and well-being through a coordinated inter/multidisciplinary team approach
- this palliative approach is conducted within a neuro-rehabilitative framework in order to achieve holistic care and support based on the needs and wishes of the person with MND and their family.
MND is a life limiting disease characterised by a series of losses with the accompanying issues of grief and bereavement which affect the patient, the carers and the family from diagnosis.
- establishing links with palliative care at an early stage can provide the primary health care team with a useful source of advice and support
- it is important that people living with MND are clear about the role of palliative care services and the benefits that they can provide.
A palliative approach needs to be integrated into the care plan for PwMND from the time of diagnosis, aiming to optimise their quality of life by relieving symptoms, providing emotional, psychological and spiritual support pre-bereavement, minimising barriers to a good death and supporting the family post-bereavement (Aoun 2018).
We have shown that survival of people attending a specialist ALS clinic has improved over a 13-year period, and that this effect is probably not fully accounted for by improvements in treatments available during that time. This supports the notion that specialist integrated multidisciplinary care provides benefit in ALS that can be measured in survival improvement.
It provides evidence that integration of palliative care services, respiratory care and wheelchair therapists, along with an MDT meeting, can improve outcomes in ALS. (Martin et al 2017).
The main aims in the care of individuals with amyotrophic lateral sclerosis (ALS) are to minimize morbidity and maximize quality of life. Although no cure exists for ALS, supportive and symptomatic care provided by a specialist multidisciplinary team can improve survival.
The basis for supportive management is shifting from expert consensus guidelines towards an evidence-based approach, which encourages the use of effective treatments and could reduce the risk of harm caused by ineffective or unsafe interventions. For example, respiratory support using non-invasive ventilation has been demonstrated to improve survival and quality of life, whereas evidence supporting other respiratory interventions is insufficient. Increasing evidence implicates a causal role for metabolic dysfunction in ALS, suggesting that optimizing nutrition could improve quality of life and survival. The high incidence of cognitive dysfunction and its impact on prognosis is increasingly recognized, although evidence for effective treatments is lacking. A variety of strategies are used to manage the other physical and psychological symptoms, the majority of which have yet to be thoroughly evaluated.
The need for specialist palliative care throughout the disease is increasingly recognized (Hobson et al 2016).
Palliative care guidelines
Shoesmith et al 2021, Canadian best practice recommendations for the management of amyotrophic lateral sclerosis: From key points: 'Palliative care and caregiver support are important components of assisting patients along their journey with ALS'. See also: table related to palliative care.
Andersen et al 2012, EFNS guidelines on the Clinical Management of Amyotrophic Lateral Sclerosis (MALS) – revised report of an EFNS task force - Palliative and end of life care recommendations:
- Whenever possible, offer input from a palliative care team early in the course of the disease.
- Initiate discussions on end‐of‐life decisions when the patient asks or provides an opportunity for discussion on the provision of end‐of‐life information and/or interventions
- Discuss the options for respiratory support and end‐of‐life issues if the patient has dyspnoea, other symptoms of hypoventilation or a forced vital capacity below 50%
- Inform the patient of the legal situation regarding advance directives and the naming of a healthcare proxy. Offer assistance in formulating an advance directive.
- Re‐discuss the patient’s preferences for life‐sustaining treatments every 6 months.
- Initiate early referral to hospice or homecare teams well in advance of the terminal phase of ALS.
- Be aware of the importance of spiritual issues for the quality of life and treatment choices. Establish a liaison with local pastoral care workers to be able to address the needs of the patient and relatives.
- For the symptomatic treatment of dyspnoea and/or intractable pain, use opioids alone or in combination with benzodiazepines if anxiety is present. Titrating the dosages against the clinical symptoms will rarely if ever result in life‐threatening respiratory depression.
- Terminal restlessness and confusion because of hypercapnia can be treated with neuroleptics.
- Use oxygen only if symptomatic hypoxia is present.
Being a syndrome with low incidence and short survival, most recommendations are good clinical practice principles (GCPPs) based on the consensus of experts in the field of ALS. Further randomized and double‐blind clinical trials are urgently needed to improve the management of ALS (Andersen et al 2012).
MND Australia is the national voice representing all Australians who share the vision of a world free of MND. MND Australia, its research arm, MND Research Australia, and members, the State MND Associations, form the only national network focused on improving the lives of all Australians living with motor neurone disease (MND) and advancing research to end MND.
MND Associations across Australia provide tailored, personalised support to people with motor neurone disease (MND) and those close to them. The support services provided may include all or some of the following:
- information
- active assistance to people living with MND, their carers and families through home visits and ongoing support
- assistance in accessing MND clinics and local services
- assistance in development of National Disability Insurance Scheme (NDIS) plans and planning
- support coordination
- provision of, and/or assistance with accessing, assistive technology
- peer support, support groups and information programs and carer workshops
- information and education for health professionals and service providers
- local advocacy and influencing
- volunteers
MND Australia is an active member of The International Alliance of ALS/MND Associations, which represents ALS/MND Associations around the world. Learn more about the MND Association in your state or territory here or call the MND Info Line on 1800 777 175.
MND clinics, located in all states and the ACT, offer outpatient services to people with MND. Specialist multidisciplinary MND Clinics usually comprise of a neurologist and other specialist doctors, nurses and allied health professionals who specialise in MND.
Referral to a neurologist at these specialist centres is recommended to confirm a diagnosis of MND.
MND clinics provide an opportunity for people with MND to see a range of health professionals for specialist and coordinated MND treatment, advice and guidance on a regular basis. Teams at MND clinics are knowledgeable about MND and provide a coordinated multidisciplinary approach to care and ongoing expert review.
The specialist MND clinics have links with other specialists, local primary health and palliative health professionals and the MND Associations in each state and territory. Clinic visits can also be supplemented by telehealth and video-conferencing, when people live at a distance or are unable to travel to clinic.
These clinics may also be available to provide specialist MND specific information and advice to support regional, rural and remote health care professionals to provide a multidisciplinary approach to care. For example the Statewide Progressive Neurological Disease (PND) Service at Calvary Health Care Bethlehem provides secondary consultation, education, and training to health professionals across the state, to support care closer to home.
Services to support people at home may be subsidised by government. A range of services can be provided and may include access to: respite, counselling, cleaning, personal care, support coordination, assistive technology and leisure and recreational activities.
There are two portals of entry to be eligible to receive subsidised services:
- National Disability Insurance Scheme (NDIS) – for people aged under 65 years
- My Aged Care – for people aged 65 years or older
MND Associations are able to advise GPs and other health professionals about local disability and aged care services, palliative care services and MND clinics. They also offer assistance to people with MND and their families to access these services. See Find services and support webpage for more information.
MND Aware e-training program MND Hub – online training course for health professionals and service providers developed by MND NSW - Session 2: MND Care approach - a person centred approach
Centre of Palliative Care, Annual Lecture 2020, Improving Palliative Care for people with neurological illness, National and International Perspectives, Dr Benzi Kluger and Dr Susan Mathers.
International ALS/MND Connect 2020:
- The MND Multidisciplinary Clinic past, present and future, Professor Chris McDermott
MND Australia, 4th MND Connect 2018:
- Multidisciplinary care and palliative care, Dr Peter Allcroft
MND Australia, 9th National MND Conference 2018:
- Motor Neurone Disease: Patient centred care for a progressive neurological disease— from ambition to reality? Dr Susan Mathers
- Until there is a cure, there is care: Integrating a palliative approach from start to end, Professor Samar Aoun
JAMA evidence, Hiroshi Mitsumoto, MD, DSc, discusses palliative care for patients with amyotrophic lateral sclerosis
Caresearch, Palliative Care Knowledge Network, Health Professionals
Resources to download
More About MND: A guide for people living with MND, their family and friendsFact sheets
Useful web pages
State MND Associations
MND Clinics
Types of help at home
How can health professionals help?


